
New Methodology for Assessing Spatial Inequality Quantitatively
24 February 2021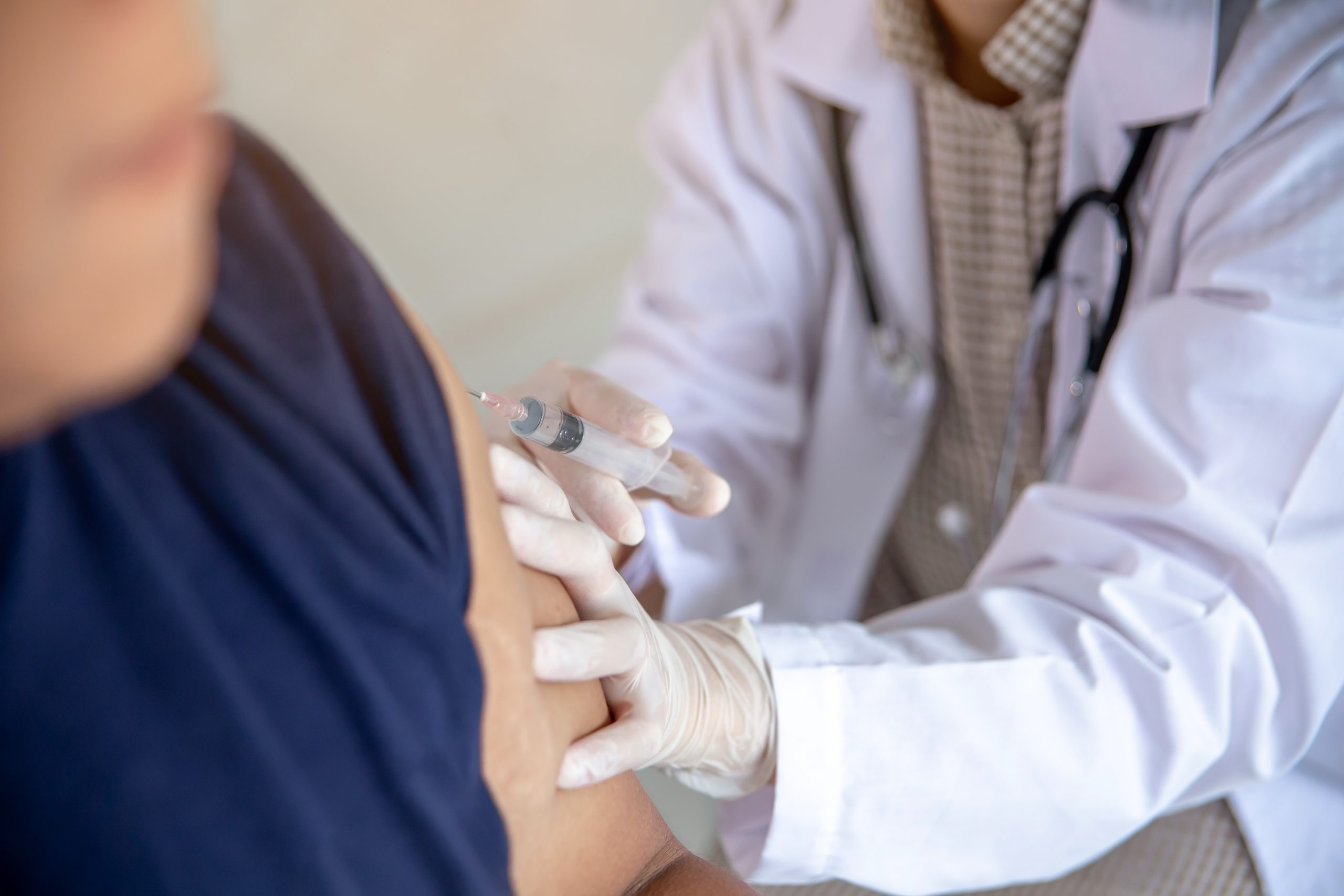
Background and trust in government affect citizens’ willingness to receive COVID-19 vaccines
25 February 2021Investigating Hong Kong Nurses’ Intention to Take Vaccines
Principal investigator: Dr Ben LI Kin-kit (Department of Social and Behavioural Sciences)

The world depends upon vaccination programmes to ease the impact of COVID-19, but it will only be effective if a considerable number of people take the vaccine. However, vaccine hesitancy, which refers to the delay in acceptance or refusal of vaccines despite the availability of vaccine services, could pose challenges to health authorities worldwide. In fact, opposition to vaccination has existed ever since the invention of the first vaccine, and it was considered a global threat by the World Health Organization in 2019.
Healthcare workers in hospitals are particularly risky during a pandemic. Protecting these people from infection plays a pivotal role in controlling nosocomial transmission. Moreover, they are a trustworthy source of vaccine information and can help build the public’s confidence in vaccination. Yet, prior research indicates that vaccine uptake rate among healthcare workers was low—the influenza uptake rate, for example, is just slightly greater than 30% among nurses in Hong Kong.
Understanding the determinants favouring vaccine uptake among nurses, therefore, could have broader policy implications for improving COVID-19 vaccination programmes acceptability and dissemination. To investigate Hong Kong nurses’ intention to have COVID-19 vaccine, Dr Ben LI Kin-kit of CityU’s Department of Social Sciences and Behavioural Sciences and his collaborators conducted a study from mid-March to late April 2020. The researcher team examined the psychological underpinnings of the vaccine hesitancy among nurses with the recently-developed 5C psychological antecedents of vaccination including confidence (trust in vaccine effectiveness, safety, and necessity and the system that delivers it), complacency (perceived the disease as low risk), constraints (perceived low vaccine availability, affordability, and accessibility), calculation (engagement in information searching), and collective responsibility (willingness to take the vaccine for protecting others via herd immunity). Work stress, which may further explain nurses’ intention to take COVID-19 vaccine, were also considered. The findings are presented in the article Influenza vaccine uptake, COVID-19 vaccination intention and vaccine hesitancy among nurses: A survey, published in the International Journal of Nursing Studies (ranked 1st in impact factor among 121 journals in nursing).
A cross-sectional online self-administered survey was conducted among nurses in Hong Kong to obtain data for the analysis. A total of 1205 responses were retained. Among all the respondents, 63% indicated that they were likely to opt for COVID-19 vaccine when available. Compared with a global-scale survey conducted in July and August 2020 that shows 74% of adults were intended to take the vaccine, Hong Kong nurses’ vaccination intention was relatively low. Younger age, stronger confidence and collective responsibility, and weaker complacency were associated with stronger intention to be vaccinated against COVID-19.
The specific COVID-19-related demands including the insufficient supply of personal protective equipment, involvement in isolated rooms and unfavourable attitudes towards workplace infection control policies were associated with greater work stress, which in turn resulted in stronger intention to have COVID-19 vaccine. Besides, the past experience of SARS contributing to strong psychological responses, as reflected in nurses’ pressure level, underlined their intention to be vaccinated against COVID-19.
Interestingly, a higher rate of nurses receiving influenza vaccine in the 2019/2020 season (49%) than in previous years was observed. It might be due to the similarity of COVID-19 symptoms to those of influenza or other respiratory diseases. Working in public hospitals, more confidence, less complacency, fewer constraints, less calculation and more collective responsibility were associated with the decision to take influenza vaccines. The results show that the 5C model was predictive of influenza vaccine uptake, and to a lesser extent, COVID-19 vaccination intention.
The study has several public health implications. First, identifying the determinants associated with COVID-19 and influenza vaccination helps inform future vaccination campaigns. For example, the study shows that older nurses are less willing to take the vaccine. But as a subgroup with high infection risk and that is likely to be the role-model of junior nurses, extra attention should be paid to protect them during future outbreaks.
Second, the uptake of safe and effective vaccine could only be considered as an additional measure to help control the COVID-19 pandemic, in view of vaccination hesitancy shown in the study. The health authority should further consider conducting modelling studies to explore the optimal levels of other interventions, such as encouragement of social distancing adoption and border controls, etc.
Third, more emphasis should be placed on psychological components when implementing nationwide vaccination programmes. Targeting the 5C components through evidence-informed interventions, health communication approaches, and new media may be viable options.
Fourth, the study shows that vaccine hesitancy is likely to be a hurdle for the uptake in Hong Kong and worldwide. The lesson learnt among nurses in Hong Kong would be helpful for the development of vaccination campaigns in the rest of the world.
Achievements and publication
Kwok, K. O.*, Li, K-K.*, WEI, W. I., Tang, A., Wong, S. Y. S., & Lee, S. S. (2021). Editor’s Choice: Influenza vaccine uptake, COVID-19 vaccination intention and vaccine hesitancy among nurses: A survey. International Journal of Nursing Studies, 114, [103854]. https://doi.org/10.1016/j.ijnurstu.2020.103854
*equal contribution
